TSC Rutherford
General, Robotic & Vascular SurgeryTSC Rutherford
515 Stonecrest Pkwy | Suite 230
Smyrna, TN 37167
TEL:615.223.9935 FAX: 615.891.5046
Mon – Fri 7:30AM – 4:30PM
General & vascular surgeons

Dr. Willie Melvin
General Surgeon
VIEW PROFILE

Dr. Joshua Taylor
General Surgeon
VIEW PROFILE

Dr. Todd Wilkens
Vascular Surgeon
VIEW PROFILE
General & vascular specialties
General & vascular Procedures
Abdominal Hernia Repair (TAR)
Achalasia Surgery
Acid Reflux Surgery
Adrenal Surgery
Anal Surgery
Anti-Reflux (GERD) Surgery
Antireflux Procedure (LINX)
Aortoiliac Occlusive Disease
Arterial Insufficiency
Atherosclerosis
Axillary Sentinel Node Biopsy
Axillary Sentinel Node Dissection
Breast Biopsy
Breast Cancer Surgery
Cancer Surgery
Carotid Bruit
Carotid Endarterectomy
Carotid Stenosis
Claudication
Colon Resection
Colon Surgery
Colorectal Surgery
Colostomy/Ileostomy Reversal
Deep Vein Thrombosis
Diagnostic Laparoscopy
Dialysis Fistulae
End Stage Renal Disease
Endocrine Surgery
Endoscopic Gastric Tube
Endoscopic Jejunal Tube
Endoscopic Placed Gastric Tube
Endoscopic Placed Jejunal Tube
Endoscopic Surgery
Excision of Lipoma
Excision of Sebaceous Cyst
Excision of Skin Cancer/Moles
Exploratory Laparotomy
Femoral to Popliteal Bypass
Femoral to Tibial Bypass
Gallbladder Surgery
Gastrectomy
Gastrointestinal Malignancy
Gastroparesis
General Surgery
HAL-RAR Surgery
Hemorrhoid Artery Ligation
Hemorrhoid Removal Surgery
Hemorrhoid Surgery
Hemorrhoidal Artery Ligation & Recto Anal Repair
Hernia Repair
Hiatal Hernia Surgery
Hyper-parathyroid surgery
Hyper-thyroid Surgery
Incisionless Hemorrhoid Surgery (HAL)
Inguinal Hernia Repair
Inguinal Hernia Surgery
IVC Filter Consult
Laparoscopic Adrenal Removal
Laparoscopic Anti Reflux Surgery
Laparoscopic Anti-Reflux Procedure (LINX)
Laparoscopic Appendectomy
Laparoscopic Cholecystectomy
Laparoscopic Colon Surgery
Laparoscopic Colorectal Surgery
Laparoscopic Colostomy
Laparoscopic Heller Myotomy
Laparoscopic Hernia Surgery
Laparoscopic Nissen Fundoplication
Laparoscopic Parastomal Hernia Repair
Laparoscopic Splenectomy
Laparoscopic Weight loss Surgery
Lipoma Removal
Liver Biopsy
Liver Surgery
Lower Extremity Ulcers
Lumpectomy
Lymph Node Biopsy
Lymphadenectomy
Mastectomy
Mesenteric Ischemia
Nissen Fundoplication
Non-Healing Wound
Pancreas Surgery
Pancreatectomy
Parathyroidectomy
Paresophageal Hernia Surgery
Peripheral Vascular Disease (PVD)
Placement of Gastric Electric Stimulator
Port-a-Cath Insertion/Removal
RAL (Robotic Assisted Laparoscopy)
RAL Colon Surgery
RAL Gallbladder Surgery
RAL Hernia Surgery
RAL Stomach Surgery
RAL Weight Loss Surgery
Rectal Surgery
Recurrent Hernia Surgery
Renal Artery Stenosis
Renal Insufficiency
Repair of Recurrent Hernias
Robotic Assisted Laparoscopic (RAL) Surgery
Robotic Colectomy
Robotic Colorectal Surgery
Robotic Hiatal Hernia Repair
Robotic Inguinal Hernia Repair
Robotic Single Site Cholecystectomy
Robotic Transversus Abdominal Release (TAR)
Robotic Ventral Hernia Repair
Scarless Parathyroid Surgery
Scarless Thyroid Surgery
Sebaceous Cyst Removal
Skin Cancer Excision
Skin Mole Excision
Small Bowel Resection
Small Bowel Surgery
Splenectomy
Splenic Artery Aneurysm
Stenting Athrectomy of Peripheral Arteries
Stomach Surgery
Subclavian Steal Syndrome
Surgical Oncology
Temporal Arteritis
Thyroid Removal
Thyroid Surgery
Thyroidectomy
Transanal Minimally Invasive Surgery (TAMIS)
Transient Ischemic Attack (TIA)
Transoral Incisionless Fundoplication (TIF)
Transoral Thyroidectomy
Transversus Abdominis Release (TAR)
Varicose Veins
Venous Insufficiency
Venous Stasis
Wound Care

Hernia Surgeons
Dr. Willie Melvin and Dr. Joshua Taylor have earned the Surgeon of Excellence in Hernia Surgery accreditation.
SURGEONS OF EXCELLENCE
SRC awarded the Hernia Surgery accreditation to Dr. Willie Melvin and Dr. Joshua Taylor after thoroughly reviewing surgical outcomes data, medical records and internal processes.
Thyroid RFA Treatments
Radiofrequency ablation (RFA) might be an option for you to discuss with your doctor. If you are a candidate, the minimally invasive thyroid treatment has many benefits:
Outpatient procedure
Utilizes local anesthesia
Low complication rate
No downtime & shorter recovery
No visible scarring
Preserves healthy thyroid tissue
No medication needed after procedure
Improves quality of life
Hemorrhoid Treatment
Why suffer from hemorrhoid pain?
Learn more about advanced hemorrhoid treatments from Dr. Melvin’s patient in this testimonial video. HAL-RAR – Hemorrhoidal Artery Ligation and Recto Anal Repair – is a new form of treatment for all grades of hemorrhoids.
How can I relieve acid reflux?
Treating GERD
Drs. Melvin and Taylor, general surgeons who specialize in GERD, answer some of the most common questions about acid reflux. This video is a great resource for anyone experiencing abnormal or consistent reflux symptoms that is looking for relief. Learn more by giving our TSC Rutherford clinic a call to schedule a consultation.
TIF Procedure in Smyrna, TN
Dr. Willie Melvin, board certified general/advanced laparoscopic/robotic surgeon at The Surgical Clinic | TSC Rutherford, speaks with Andrea Millers from EndoGastric Solutions about anti-reflux (GERD) procedures known as TIF. *GERD – GastroEsophageal Reflux Disease, also referred to as acid reflux or heartburn.
Learn more about what GERD is and what types of symptoms patients can typically feel if they’re suffering from GERD or acid reflux.
Who should get a vascular screening?
Vascular health screenings should be considered for those who meet one or more of the following:
50 years or older
Current or previous smoker
High cholesterol
High blood pressure
Diabetes
Family history
About TSC Rutherford
TSC Rutherford is a proud partner of The Surgical Clinic with a focus on general surgery, robotic surgery, hernias, GERD, and vascular surgery. Our board certified general & vascular surgeons specialize in a range of advanced and complex procedures that include transoral incisionless fundoplication (TIF), HAL-RAR, scarless thyroid and parathyroid surgery, along with many other procedures.
Robotic Hernia Repair
Robotic Heria Repair (TAR)
Did you know the first robotic hernia repair was performed in Tennessee by our very own Dr. Joshua Taylor at TriStar StoneCrest?
Dr. Melvin and Dr. Taylor are regional leaders for robotic hernia surgery.
Dr. Taylor was first to perform a transversus abdominus release (TAR) w/ robotic surgery in Tennessee. Dr. Melvin and Dr. Taylor both perform complex hernia repairs, re-operative and recurrent hernia repairs, and “component separations” with the robotic approach. The robotic procedure adds reinforcement to the abdominal wall to prevent the recurrences or other hernias from developing, recovers the abdominal wall functionality, prevents the intra-abdominal organs from protruding through the abdominal wall and provides a cosmetically-pleasing appearance.
Patient results:
- quicker discharge
- less pain
- quicker return to normal activities
Robotic surgery has been demonstrated to have fewer complications for inguinal hernia surgery.
(Surgical Endoscopy 2017)
Learn more about this advanced ventral hernia repair in this short video.
Patients with Rectal Polyps
TAMIS
Dr. Melvin and Dr. Taylor are the only certified TAMIS surgeons in the Rutherford county area.
(https://tamissurgery.com/find-a-surgeon search Tennessee)
Minimally invasive approach to treating rectal polyps and even early stage rectal tumors.
“By combining local excision techniques and chemoradiation, the problem of persistent disease from untreated lymphatics is addressed. In higher lesions, TEM/TAMIS helps address the problem of specimen fragmentation and the challenge of achieving clear margins by operating with an endoluminal approach. With the combination of these approaches, the patient has an increased chance for success with an expanded role of local therapy for stage I rectal cancer.” Complexities in Colorectal Surgery 2014
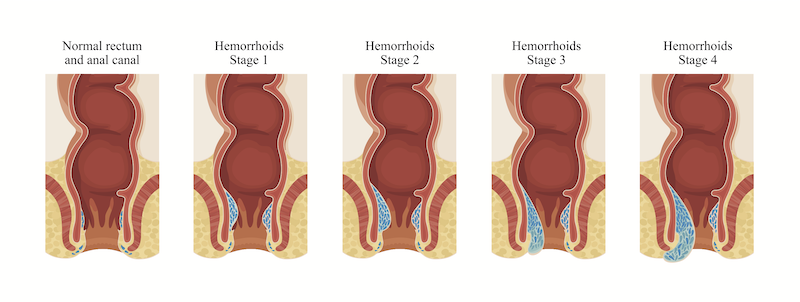
Incisionless Hemorrhoid Surgery (HAL-RAR)
HAL-RAR
Hemorrhoidal Artery Ligation and Recto Anal Repair (HAL-RAR)– is a new form of treatment for all grades of hemorrhoids. Some 50% of people will suffer from hemorrhoidal disease at some stage in their life, however up until now, many of them have put off consulting their doctor because of the pain associated with the various treatment methods
The ligations serve to reduce the arterial blood supply, causing the haemorrhoidal cushions to shrink back to normal size. The HAL-RAR method is used to treat the prolapsing hemorrhoids that occur during more advanced stages of the disease. HAL-RAR involves one or more mucopexies of prolapsing mucosa, carried out after the hemorrhoidal arteries have been ligated. All of this is performed through the anus and is incisionless. This has been shown to be effective and result in high patient satisfaction!
Noninvasive Hernia Surgery
Robotic Hernia
Dr. Melvin and Dr. Taylor are regional leaders for robotic hernia surgery.
Dr. Taylor was first to perform a transversus abdominus release (TAR) w/ robotic surgery in Tennessee. Dr. Melvin and Dr. Taylor both perform complex hernia repairs, re-operative and recurrent hernia repairs, and “component separations” with the robotic approach. The robotic procedure adds reinforcement to the abdominal wall to prevent the recurrences or other hernias from developing, recovers the abdominal wall functionality, prevents the intra-abdominal organs from protruding through the abdominal wall and provides a cosmetically-pleasing appearance.
Patient results:
- quicker discharge
- less pain
- quicker return to normal activities
Robotic surgery has been demonstrated to have fewer complications for inguinal hernia surgery.
(Surgical Endoscopy 2017)
Heartburn & GERD Symptoms
Heartburn is discomfort or actual pain caused by digestive acid moving into the tube that carries swallowed food to your stomach (esophagus).
Do you have a burning pain in your chest, just behind your breastbone?
Is the pain worse after eating, in the evening, or when lying down or bending over?
Do you have a burning feeling in your throat?
Do you experience a bitter or acidic taste in the mouth?
Have you experiences a long-term cough, sore throat, or hoarseness?
How is GERD diagnosed?
Heartburn/GERD Diagnosis
Welcome to the 4th facebook live session of “Is your heartburn something more serious?” with Dr. Joshua Taylor, board certified general surgeon with The Surgical Clinic.
Treatment options for heartburn or GERD: lifestyle changes, medications or surgery.
65%-75% of patients manage thier heartburn and GERD symptoms with lifestyle changes and medications.
When lifestyle and medication are not enough, your provider may order additional testing:
Reflux Testing
High-Resolution Manometry
Motility Testing
X-Rays
Endoscopy
What is Scarless Thyroid Surgery?
Scarless Thyroid and Parathyroid Surgery
The Surgical Clinic (TSC) specializes in advanced technologies for giving patients the best results possible and proudly offers a scarless approach to thyroid surgery called a transoral thyroidectomy. Transoral simply means through the mouth. This particular procedure is performed by Dr. Joshua Taylor, a board certified general surgeon with TSC Rutherford, who performs thyroid and parathyroid surgery through the lip to alleviate scarring post surgery. Dr. Taylor was trained at Johns Hopkins hospital, which has had the most experience performing the transoral approach to thyroid and parathyroid surgery since 2015. In the past 5 years, medical experts have completed over 3,000 studies to prove this successful approach to be safe and effective.
Many patients prefer this newer, advanced approach to prevent having a scar on their neck after surgery. To learn more about scarless thyroid surgery, Dr. Taylor explains the benefits, studies, potentials complications and more in the video below.
Colon, Rectal & Anal problems
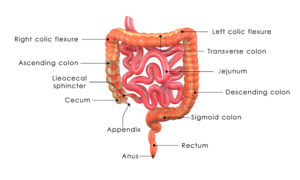
Colorectal Surgery
Our standard is minimally invasive surgery with proven results. Minimally Invasive approach to colorectal surgery is not the standard approach. 75% of colorectal surgery nationally is performed open! 75% of our patients underwent a laparoscopic or robotic colorectal surgery NOT open! In 2016, The Johns Hopkins Hospital published its data on colorectal procedures.They reported a median length of stay of EIGHT days in the hospital. Our median length of stay is 5 days for laparoscopic and 4.5 for robotic surgery!
Revolutionary Solutions for Reflux - LINX®
LINX® Reflux Management System
Unlike other procedures to treat reflux, LINX is implanted around the outside of the Lower Esophageal Sphincter (LES) and requires no alteration to the stomach.
LINX preserves normal physiological function so you can belch or vomit as needed. The titanium beads open and close to let food down, and if it needs to come up, it can.
The device will not affect airport security. And you can still have an MRI. Enjoy life with LINX.
Reflux sufferers, meet LINX® — a revolutionary solution for reflux. It’s a simple device with life-changing potential. LINX is intended for patients diagnosed with Gastroesophageal Reflux Disease (GERD) as defined by abnormal pH testing, and who are seeking an alternative to continuous acid suppression therapy. Continue on to learn more about this small device with big results.
Gastroesophageal Reflux Disease or GERD is a condition in which fluids from the stomach wash back into the Esophagus.
GERD is more than just a nuisance. Over time, the repeated exposure to stomach acids can cause permanent damage to the Esophagus and can even result in cancers. When medications aren’t working, surgery is an option and there is a new surgical procedure called LINX that offers patients a less invasive procedure.
LINX is a procedure that allows the Surgeon to place a beaded necklace made of magnets around the weakened valve area of the Esophagus. These magnets help the valve to stay closed, but can flex when the valve needs to open to allow food to head to the stomach. LINX allows patients to often go home the day of the surgery and begin eating a regular diet right away. Should there ever be a reason to remove the LINX necklace, it can be done in a minimally invasive way and the necklace leaves no permanent change to the Esophagus itself.
If you are suffering from Reflux problems that don’t respond to medication, LINX may be your best move.
GERD symptoms
GERD FAQ
Welcome to the 2nd facebook live session of “Is your heartburn something more serious?” with Dr. Joshua Taylor, board certified general surgeon with The Surgical Clinic.
What is heartburn or GERD?
Heartburn/GERD is a chronic condition in which acid from your stomach flows back into your esophagus (the swallowing tube). That acid begins to cause damage to the lining of the esophagus and that causes pain. This is where the reflux definition comes from.
What are the symptoms you can experience from heartburn or GERD?
- difficulty swallowing, also known as dysphagia
- painful swallowing, also known as odynophagia
- dry throat
- sore throat
- feeling of a lump in your neck, referred to as globus sensation
- vomiting or regurgitation
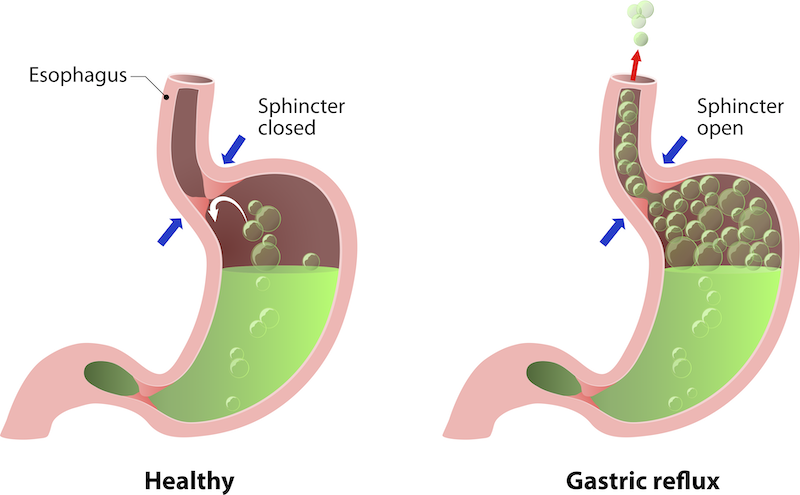
What causes heartburn/GERD/reflux?
GERD or reflux is caused by temporary or sometimes permanent changes in the barrier between the esophagus and the stomach. When the lower part of the esophagus, known as the sphincter, is closed no acid can reflux up. However, if the sphincter is open or becomes incompetent, acid can constantly reflux up. Another cause of reflux is if you have a hiatal hernia. Learn more about GERD treatment in Rutherford County from Dr. Joshua Taylor and Dr. Willie Melvin during their live facebook series.
How to manage gerd
Heartburn FAQ
Welcome to the 1st in a series of seminars with Dr. Melvin! Today’s focus is on heartburn – “Is your heartburn something more serious?“
What is heartburn?
Heartburn is a term commonly used to describe symptoms. Most of the burning sensation is the epigastric, or upper abdomen area next to the heart. A lot of patients come in and present to the emergency room with symptoms similar to a heart attack. It goes by the name of heartburn, indigestion, reflux, acid reflux… All of those describe the symptoms presented from the regurgitation of acid from the stomach to the esophagus.
How do you manage heartburn? Initially, symptoms may present once or twice after a certain event or after certain meals, sometimes we overindulge at Thanksgiving and all of that pressure forces more acid up. The reality is that all of us have reflux; it’s a normal physiological response. The difference is that normally once you get that reflux, there’s an inherent mechanism that flushes away (or neutralizes/clears away) that process. In the standing position, if you have reflux, acid would then go down because of gravity. The alkaline nature of your saliva as you swallow, it neutralizes some of that reflux. The normal valve mechanism that causes things to go in one direction sometimes doesn’t work well and that presents with a pathologic problem of acid reflux disease, heartburn, or GERD (gastroesophageal reflux disease).
Initially, once heartburn has been treated, sometimes you can get medicines over the counter. A lot of these are more powerful, anti-acid or acid blocking medicine, which is okay once in awhile.
How to reduce initial heartburn: adjust your diet, don’t over eat, have smaller portions over a day period, modify your behavior, don’t eat too late and then lay down. Learn more about what heartburn is and how to treat it from Dr. Melvin.
TIF for Reflux
TIF is an acronym, transoral incisionless fundoplication, and the advantage is that it is ‘surgery from within’ performed through the mouth, not through an incision. TIF procedure with the EsophyX device is a simple intervention that repairs the gastroesophageal valve, the root cause of GERD. The TIF procedure reconstructs the valve between the esophagus and the stomach to prevent reflux.
The FDA approved this device and procedure in 2007.
Minimally invasive: Fast recovery
Restores valve to natural state: Maintain normal bodily functions
No incisions: No scars
No metal implant: No need to remove foreign object
No dissection of stomach: No scar tissue
Clinical studies show that at three years after the TIF procedure:
70% were able to completely stop PPI therapy
87% of patients reported reflux esophagitis healed
91% of patients reported elimination of troublesome regurgitation
Referring physicians
Referring to TSC Rutherford ensures your patient receives exceptional surgical care, compassionate concern, and access to the most technologically advanced surgical practice in Smyrna and Murfreesboro.
Why Choose Us
Experienced Doctors
TSC Rutherford has 3 board certified general & vascular surgeons with clinical & business staff who are dedicated to serving our referring physicians & their patients in Tennessee.
ADVANCED PROCEDURES
Dr. Willie Melvin & Dr. Joshua Taylor specialize in Robotic Assisted Laparoscopic (RAL) procedures & advanced incisionless techniques.