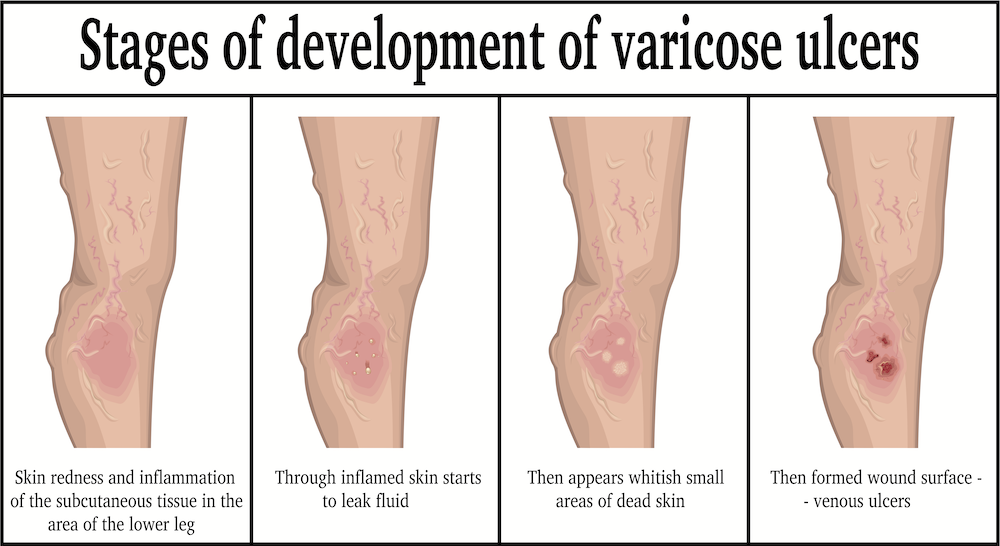
As vascular surgeons who specialize in the treatment of veins and arteries, many patients will reach us having had a series of leg ulcers which have taken long times to heal and have required them to wear uncomfortable and hard to wear compression stockings in the hopes of healing one after another ulcer.
Traditionally, patients with postphlebitic legs and venous stasis ulcers have been treated with compression wraps for ulcer healing and long term stockings to prevent a recurrence. Compliance with stockings is very poor, particularly in the hotter months. Stasis ulcer recurrence rates are very high. Each successive episode results in more scarring. Symptoms worsen over time and can result in permanent disability.
The new onset of swelling of a single leg has traditionally been labeled lymphedema. Ultrasound fails to adequately see the iliac veins or inferior vena cava in all but the thinnest of patients. Again, for lymphedema, the best long-term treatment was compression therapy. In fact, many patients have compression of the iliac vein between the overlying artery and the lumbar spine. This condition, known as May Thurner syndrome, is more common on the left side and maybe the underlying reason why DVT is more common in the left leg. May Thurner can occur in the right leg as well.
Related: Peripheral Arterial Disease: Don’t Ignore It
Several published series in recent years culminated in an evidence summary in the Journal of Vascular Surgery in 2013. Fifteen hundred patients were followed for three to five years after venography and balloon and stenting of significant iliac vein or IVC stenoses. Procedural success was achieved in nearly 100% of stenosis and 83-95% of occlusions. Morbidity, including DVT, occurred in less than 1% of patients. Three to five-year patency was 90-100% in non-thrombotic patients and 74-89% in post-thrombotic patients. Significant pain relief was experienced by 86-94% of patients and swelling improved considerably in 66-89%. In patients not already on permanent anticoagulation, postprocedural anticoagulation for 30 days followed by daily 81 mg aspirin is generally used.
Our experience in treating deep vein stenoses approaches 100 patients over the last two years. Though follow-up is short, significant clinical improvement has been achieved in a large majority of patients, some of whom had had leg swelling for over twenty years. Complications have been low, similar to the published results above. A typical postphlebitic case is shown.
Future areas of research in deep vein stenosis include the type and length of anticoagulation needed, effectiveness (and reimbursement) of intravascular ultrasound for diagnosis and treatment, and development of new stents specifically designed for veins.

Dr. Julia Boll
Vascular Surgeon
VIEW PROFILE

Dr. Jeffery B. Dattilo
Vascular Surgeon
VIEW PROFILE

Dr. JimBob Faulk
Vascular/Endovascular Surgeon
VIEW PROFILE

Dr. Bryan T. Fisher
Vascular Surgeon
VIEW PROFILE

Dr. Brian Kendrick
Vascular Surgeon
VIEW PROFILE

Dr. Billy J. Kim
Vascular Surgeon
VIEW PROFILE

Dr. Allen Lee
Vascular Surgeon
VIEW PROFILE

Dr. Caroline Nally
Vascular Surgeon
VIEW PROFILE

Dr. Adam Richter
Vascular/Endovascular Surgeon
VIEW PROFILE

Dr. Mark Shelton
Vascular Surgeon
VIEW PROFILE

Dr. Todd H. Wilkens
Vascular Surgery
VIEW PROFILE

Dr. Patrick Yu
Vascular Surgeon
VIEW PROFILE