Podiatry
FOOT AND ANKLE TREATMENT THROUGHOUT MIDDLE TENNESSEE
The Surgical Clinic is your premier destination for expert foot and ankle care in Nashville, Mt. Juliet, and Lebanon, TN. As dedicated foot specialists, we address a wide range of conditions, from common foot problems to specialized surgical interventions. Trust our skilled podiatrists to provide personalized solutions for your unique needs.
What is podiatry?
Podiatry, also known as chiropody, is a specialized branch of medicine focusing on the diagnosis and treatment of foot, ankle, and lower leg disorders. Our healthcare professionals, referred to as podiatrists or Doctors of Podiatric Medicine (DPM), are committed to ensuring your feet receive the best care possible.
Conditions We Treat
Our podiatrists in Nashville are equipped to treat a diverse range of foot and ankle problems, including arthritis, bunions, hammertoes, plantar warts, and even conditions related to diabetes and obesity. From ingrown toenails to complex injuries, our podiatry clinic is your comprehensive solution for foot and ankle ailments for the whole family.
What does a podiatrist do?
Podiatrists are also known as DPMs (Doctors of Podiatric Medicine). Podiatrists handle almost everything below the knee, like the lower leg, foot, and ankle. They are able diagnose and treat diseases, disorders, and injuries with specialized care. They also prescribe medications and orthotics, perform physical therapy services, and administer surgery when needed.
The main responsibilities and services provided by podiatrists include:
Diagnosing Foot and Ankle Conditions
Treating Foot and Ankle Conditions
Managing Foot and Ankle Injuries
Addressing Foot Deformities
Providing Diabetic Foot Care
Performing Foot and Ankle Surgeries
Prescribing Custom Orthotics
Conducting Gait Analysis
Treating Sports-Related Injuries
Educating Patients
Overall, podiatrists are essential healthcare professionals who focus on the health and well-being of the feet and lower extremities, helping patients maintain mobility, alleviate pain, and improve their overall quality of life.
Our foot surgeons at The Surgical Clinic specialize in various procedures, utilizing advanced techniques to alleviate discomfort and enhance mobility. The dedicated team of skilled podiatrists ensures exceptional foot and ankle care, addressing pain, injuries, and various conditions affecting the lower extremities. Combining their expertise with personalized treatment plans, our podiatrists strive for optimal outcomes, whether dealing with Achilles tendon pain, ankle sprains, or the need for joint replacement. Regardless of the podiatric condition, our doctors bring extensive experience and knowledge, providing a comprehensive range of services from routine check-ups to advanced surgical interventions, offering a holistic approach tailored to your specific needs.
PODIATRISTS
Dr. Timothy W. Bush, DPM
Foot & Ankle Specialists
4230 Harding Pike | Suite 202
Nashville, TN 37205
TEL: 615.662.6676 FAX: 615.662.8371
Mon – Thur 8AM – 5PM
Fri 8AM – 12PM
Dr. Tod Bushman, DPM
Lebanon Clinic
920 S. Hartmann Rd. | Suite 340
Lebanon, TN 37090
TEL: 615.784.4039 FAX: 615.871.9682
Mon – Fri 7:30AM – 4:30PM
Summit Clinic
660 S. Mt. Juliet Rd. | Suite 230
Mt. Juliet, TN 37122
TEL: 615-874-9667 FAX: 615.871.9682
Mon – Fri 7:30AM – 4:30PM
Common foot & ankle problems in podiatry
Bunions
Bunions are misaligned big toe joints that swell and become tender, causing the first joint of the big toe to slant outward and the second joint to angle toward the other toes. Bunions tend to be hereditary but can be aggravated by shoes that are too narrow in the forefoot and toe. Surgery is frequently performed to correct the problem.
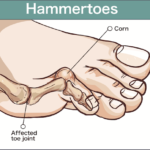
Hammertoes
Hammertoes usually stemming from muscle imbalance, this condition occurs when the toe is bent into a claw-like position. Hammertoe can affect any toe, but most frequently occurs to the second toe, when a bunion slants the big toe toward and under it. Selecting shoes and socks that do not cramp the toes may help alleviate any aggravation of pain or discomfort.
Heel Spurs
Heel Spurs—growths of bone on the underside, forepart of the heel bone. Heel spurs occur when the plantar tendon pulls at its attachment to the heel bone. This area of the heel later calcifies to form a spur. Proper warm-up and the use of appropriate athletic shoes can reduce the strain to the ligament and prevent the formation of heel spurs.
Ingrown Toenails
Ingrown Toenails are toenails with corners or sides that dig painfully into the skin. Ingrown toenails are usually caused by improper nail trimming, but can also result from shoe pressure, injury, fungus infection, heredity, and poor foot structure. Women are more likely to have ingrown toenails than men. The problem can be prevented by trimming toenails straight across, selecting proper shoe styles and sizes, and responding to foot pain in a timely manner.
If the ingrown toenail becomes severe, a food doctor may need to remove the ingrown toenail.
Neuromas
Neuromas—enlarged benign growths of nerves, most commonly between the third and fourth toes. Neuromas are caused by tissue rubbing against and irritating the nerves. Pressure from ill-fitting shoes or abnormal bone structure can also lead to this condition. Depending on the severity, treatments may include orthotics (shoe inserts), cortisone injections, and, in extreme cases, surgical removal of the growth.
Plantar Fasciitis
Plantar Fasciitis is an inflammation on the bottom of the foot that leads to heel and arch pain. Various foot injuries or improper foot mechanics can lead to plantar fasciitis. Treatments range from icing and foot exercises to prescription custom orthotics to correct the foot position and help alleviate pain.
Plantar Wart
Plantar warts, caused by the human papillomavirus (HPV), are growths that appear on the soles of your feet. These often uncomfortable lesions can make walking a painful experience. Our skilled podiatrists at The Surgical Clinic offer a range of effective treatments, from topical medications to freezing and laser therapy, ensuring a targeted approach to remove plantar warts and restore comfort to your steps.
Shin Splints
Shin Splints—pain on either side of the leg bone caused by muscle or tendon inflammation. Shin splints are related to excessive foot pronation, but also may be related to a muscle imbalance between opposing muscle groups in the leg. Proper stretching before and after exercise and corrective orthotics for pronation can help prevent shin splints.
Sesamoiditis
Sesamoiditis—an inflammation or rupture of the two small bones (known as sesamoids) under the first metatarsal bone. Proper shoe selection and orthotics can help.
Stress Fractures
Stress Fractures—incomplete cracks in bone caused by overuse. With complete rest, stress fractures in toes or any bones of the foot heal quickly. Extra padding in shoes can help prevent the condition. Left untreated, stress fractures may become complete bone fractures, which require casting and immobilization.
When to consult a foot doctor
Persistent foot or ankle pain is not normal. Recognize the signs and consult a podiatrist if you experience:
- Persistent pain in your feet or ankles
- Ankle instability
- Changes in toenails or skin on your foot
- Ingrown toenails
- Severe cracking, scaling, or peeling on the heel or foot
- Increased pain, swelling, redness, tenderness, or heat
- Foot, ankle, or lower leg injuries
- Red streaks extending from the affected area
- Symptoms from diabetes, like poor circulation and Athlete’s Foot
Trust The Surgical Clinic to connect you with a foot doctor in Nashville to address these conditions promptly.if necessary, our podiatrists can perform surgery as part of treatment.
Podiatry Services We Offer
Foot and Ankle Examinations:
Our podiatrists perform thorough examinations to diagnose the root cause of your foot and ankle issues. Physical assessments, imaging techniques, and diagnostic tests help uncover underlying factors contributing to discomfort.
Conservative Treatments:
In many cases, non-invasive treatments can effectively manage podiatric conditions. We use conservative approaches, like orthotics, bracing, physical therapy, and medication, to relieve pain, reduce inflammation, and promote healing.
Minimally Invasive Procedures:
We also offer a range of minimally invasive procedures to address specific foot and ankle conditions. Advanced techniques like ultrasound-guided injection and laser therapy minimize scarring, reduce recovery time, and provide excellent outcomes.
Surgical Interventions:
If your condition requires surgical intervention, our skilled podiatrists have extensive expertise in performing a wide array of foot and ankle surgeries, from bunionectomy and hammertoe correction to ankle arthroscopy and ligament repair.
Diabetic Foot Care:
For individuals with diabetes, proper foot care is essential to prevent complications such as foot ulcers and infections. Our diabetic podiatry specialists offer regular examinations, wound management, and education on preventive measures to maintain optimal foot health.
Comprehensive podiatry procedures and treatments
Achilles Tendon Pain
Ankle Pain & Instability
Ankle Sprains
Arthritis
Athletes Foot
Bunions
Pediatric podiatry
Corns & Calluses
Crush Injuries
Diabetic Foot Care
Flat Feet
Fractures
Fungus Toenails
Geriatric Foot Care
Hammertoes
Heel Pain
Heel Spurs
Ingrown Toenails
Infected Toe
Injuries
Joint Replacement
Neuromas (Pinched Nerve)
Orthotics
Plantar Fasciitis/Heel Pain Treatment
Plantar Warts
Reconstructive Surgery
Sports Podiatry – Injury treatment
Toe injuries
Warts
Nashville Podiatry Specialties at TSC
Achilles Surgery
Surgery to repair a torn (ruptured) Achilles tendon is conducted on an outpatient basis using a local anesthetic. It involves making an incision or cut in the back of the leg above the heel to access the torn tendon. The tendon is then sewn back together. Surgery may be delayed for about one week after the rupture to let the swelling go down.
After surgery, patients usually wear a cast or walking boot for six to 12 weeks. At first, the cast or boot is positioned to keep the foot pointed downward as the tendon heals. The cast or boot is then adjusted gradually to put the foot in a neutral position (not pointing up or down).
Specific gentle exercises (restricted motion) after surgery can shorten the time needed in rehabilitation.
Ankle Surgery
Ankle surgery may be required to correct a serious deformity of the ankle and its bone structure. Injury (such as a fracture), birth defects, or changes throughout the course of life are the usual culprits. Diseases, such as diabetes, rheumatoid arthritis, and neuromuscular conditions, may cause severe foot and ankle deformities that, over time, cause pain and difficulty in walking.
Ankle surgeries emphasize the realignment of the structure either around or after removal of the deformity. Various kinds of internal and external fixation devices—some temporary, others permanent—are often required to maintain the appropriate alignment during, and beyond, the healing process.
Ankle surgeries vary in complexity, length, and severity, yet many of them today are conducted on a same-day, outpatient basis. Patients need to arrange for another person to take them home afterwards and stay with them for the first 24 hours following the surgery. Post-operative instructions, provided by your surgeon, will give you the information needed to care for your recovering ankle following surgery.
Arthritis Surgery
Patients who undergo surgery to correct arthritis in the foot are often diabetics with a type of arthritis known as Charcot Foot. The average age of patients developing a Charcot foot is 40 years. About one-third of patients develop a Charcot foot in both feet and/or ankles. This form of arthritis can develop suddenly and without pain. Quite suddenly, the bones in the foot and/or ankle can spontaneously fracture and fragment, often causing a severe deformity.
The arch of the foot often collapses, and pressure areas develop on the bottom of the foot, leading to open sores or ulcers.
While many of these deformities can be treated with nonsurgical care, surgery may be required. Such instances may include:
- Chronic deformity with increased plantar pressures and risk of ulcers.
- Chronic deformity with significant instability that cannot be corrected by braces.
- Significant deformity that may include ulcers that don’t heal or respond to therapy.
Surgical procedures used to treat arthritis include:
- Hindfoot and ankle realignment. This kind of procedure is usually prescribed when there is significant instability resulting in a patient being unable to walk. Various types of internal fixation are placed within the foot during this kind of procedures.
- Midfoot realignment. This kind of procedure is usually prescribed when there is significant instability of the middle portion of the foot. During a midfoot realignment, various types of internal fixation are placed within the foot.
- Ostectomy. In this procedure, a portion of bone is removed from the bottom of the foot. It is usually performed for a wound on the bottom of the foot that is secondary to pressure from a bony prominence.
Bunions
Bunions
A bunion is a bone deformity caused by an enlargement of the joint at the base and side of the big toe (metatarsophalangeal joint). Bunions form when the toe moves out of place. The growth and its protuberance cause friction and pressure as they rub against footwear. Over time, the movement of the big toe angles toward the other toes, sometimes overlapping a third toe (known as Hallux Valgus). The growing enlargement or protuberance then causes more irritation or inflammation. Sometimes, the big toe moves toward the second toe and rotates or twists, known as Hallus Abducto Valgus. Bunions can also lead to other toe deformities, such as hammertoe.
Many people with bunions suffer from discomfort and pain from the constant irritation, rubbing, and friction of the enlargement against shoes. The skin over the toe becomes red and tender. Because this joint flexes with every step, the bigger the bunion gets, the more it hurts to walk. Over time, bursitis or arthritis may set in, the skin on the bottom of the foot may become thicker, and everyday walking may become difficult—all contributing to chronic pain.
Heredity is the leading cause of bunions, usually because of a faulty foot structure. In addition, foot injuries, neuromuscular problems, flat feet, and pronated feet can cause bunion formation. It is estimated that bunions occur in 33 percent of the population in Western countries. Wearing tight-fitting shoes can aggravate the deformity but does not cause bunions.
Treatment for Bunions
Because they are bone deformities, bunions do not resolve by themselves. The goal of bunion treatment is to relieve the pressure and pain caused by irritations and to stop any progressive enlargement growth. Commonly used methods for reducing pressure and pain caused by bunions include:
- The use of protective padding, often made from felt material, eliminates the friction against shoes and helps alleviate inflammation and skin problems.
- Remove foot corns and calluses.
- Switch to carefully-fitted footwear designed to accommodate the bunion and not contribute toward its growth.
- Use Orthotic devices—over-the-counter and custom-made—to help stabilize the joint and place the foot in the correct position for walking and standing.
- Exercise to maintain joint mobility and prevent stiffness or arthritis.
- Wear splints for nighttime use to help the toes and joints align correctly. Splints are often recommended for adolescents with bunions because their bone development may still be adaptable.
Surgical Bunion Treatment
Depending on the size of the enlargement, misalignment of the toe, and pain experienced, conservative treatments may not be adequate to prevent progressive damage from bunions. In these cases, bunion surgery, known as a bunionectomy, may be advised to remove the bunion and realign the toe.
Cyst Removal
Ganglion masses, or cysts, are normally removed through surgery. Most cyst removal surgeries are performed on an outpatient basis. Contact our office to have this procedure performed.
During the procedure, the cyst is dissected from the surrounding soft tissues and removed. The recovery period depends on the location of the ganglion and the amount of dissection required during surgery. In many cases, patients receive a splint or below-the-knee cast. The surgeon may require the patient to use crutches for several days to up to three weeks. This level of protection may be necessary if the ganglion is near the ankle joint.
Possible complications from cyst removal surgery include infection, excessive swelling, and nerve damage.
Flatfoot correction
Adult-acquired flatfoot or posterior tibial tendon dysfunction usually leads to a gradual loss of the arch. The posterior tibial muscle is a deep muscle in the back of the calf and has a long tendon that extends from above the ankle and attaches into several sites around the arch of the foot. The muscle acts like a stirrup on the inside of the foot to help support the arch. The posterior tibial muscle stabilizes the arch and creates a rigid platform for walking and running. If the posterior tibial tendon becomes damaged or tears, the arch loses its stability and as a result, collapses, causing a flatfoot.
Surgery is often performed to give the patient a more functional and stable foot. Several procedures may be required to correct a flatfoot deformity, depending on the severity of the problem. These may include:
- Tenosynovectomy—a procedure to clean away (debridement) and remove any of the inflamed tissue around the tendon.
- Osteotomy—removal of a portion of the heel bone (calcaneus) to move the foot structure back into alignment.
- Tendon Transfer—in which replacement fibers from another tendon are inserted to help repair damage.
- Lateral Column Lengthening—A procedure that implants a small piece of bone, usually removed from the hip, outside of the heel bone to create the proper bone alignment and rebuild the arch.
- Arthrodesis—Fusing of one or more bones together to eliminate any joint movement, which stabilizes the foot and prevents any further deterioration or damage.
Ingrown Toenails
Ingrown toenails, also known as onychocryptosis, is usually caused by trimming toenails too short, particularly on the sides of the big toes. They may also be caused by shoe pressure (from shoes that are too tight or short), injury, fungus infection, heredity, or poor foot structure. Ingrown toenails occur when the corners or sides of the toenail dig into the skin, often causing infection. A common ailment, ingrown toenails can be painful. Ingrown toenails start out hard, swollen, and tender. Left untreated, they may become sore, red, and infected and the skin may start to grow over the ingrown toenail.
Ingrown Toenail Surgery and Treatment
In most cases, ingrown toenail treatments are simple: soak the foot in warm, soapy water several times each day. Avoid wearing tight shoes or socks. Antibiotics are sometimes prescribed if an infection is present. Note: Please consult your physician before taking any medications. In severe cases, if an acute infection occurs, surgical removal of part of the ingrown toenail may be needed. Known as partial nail plate avulsion, the ingrown toenail removal involves injecting the toe with an anesthetic and cutting out the ingrown part of the toenail.
You can prevent ingrown toenails by:
- Trimming toenails straight across with no rounded corners.
- Ensuring that shoes and socks are not too tight.
- Keeping feet clean at all times.
Hammertoe Surgery
Hammertoe is a deformity of the second, third, or fourth toes. In this condition, the toe is bent at the middle joint, causing it to resemble a hammer. Left untreated, hammertoes can become inflexible and painful, requiring surgery.
Hammertoe surgery can be done on an outpatient basis in the doctor’s office or a surgery center using a local anesthetic, sometimes combined with sedation. The surgery takes about 15 minutes to perform. Up to four small incisions are made and the tendons are rebalanced around the toe so that it no longer curls. Patients usually can walk immediately after the surgery wearing a special surgical shoe. Minimal or no pain medication is needed following the surgery.
Icing and elevation of the foot is recommended during the first week following the procedure to prevent excessive swelling and promote healing. It is also important that the dressing be kept clean and dry to prevent infection. Two weeks after the surgery, the sutures are removed and a wide athletic shoe can replace the post-operative surgical shoe. Patients can then gradually increase their walking and other physical activities.
Heel pain
Heel Pain Treatment in Nashville
Plantar fasciitis is the term commonly used to refer to arch and heel pain traced to an inflammation on the bottom of the foot. More specifically, plantar fasciitis is an inflammation of the connective tissue, called plantar fascia, that stretches from the base of the toes, across the arch of the foot, to the point at which it inserts into the heel bone. Overpronation is the most common cause of plantar fasciitis. As the foot rolls inward excessively when walking, it flattens the foot, lengthens the arch, and puts added tension on the plantar fascia. Over time, this causes inflammation.
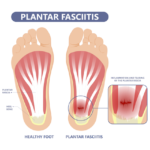
Also known as heel spur syndrome, the condition is often successfully treated with conservative measures, such as the use of anti-inflammatory medications, ice packs, stretching exercises, orthotic devices, and physical therapy. Note: Please consult your physician before taking any medications.
Meet Our Board-Certified Podiatrists

Dr. Timothy Bush
Podiatrist
VIEW PROFILE

Dr. Tod Bushman
Podiatrist
VIEW PROFILE
The Podiatry Division at The Surgical Clinic
The Surgical Clinic podiatry branch is your answer to all podiatry/foot and ankle-related questions and needs. So whether you sprained your ankle, have a pinched nerve, or you’re looking for expert diabetic foot care, we have a podiatrist ready to help.
Choosing a Podiatrists in Tennessee
Our board-certified podiatrists, Dr. Timothy W. Bush and Dr. Tod Bushman bring a wealth of experience to our Nashville and Lebanon clinics. They are dedicated foot and ankle specialists, offering compassionate care and personalized treatment plans to address your specific needs.
Both Drs. Bush and Bushman are long-standing American Podiatric Medical Association members and board-certified podiatrists. They are your dream team for family foot care in Nashville.
See a Podiatrist in Nashville
Looking for a foot & ankle specialist or podiatrist in Nashville?
Our board-certified podiatrists, who specialize in foot and ankle surgery, strive to offer our patients the best podiatry treatments and procedures in Nashville, Mt. Juliet, Lebanon, and throughout Middle Tennessee.
Our podiatrists at The Surgical Clinic in Tennessee can treat injuries, diagnose diseases, and help patients manage ongoing foot, ankle, and leg issues resulting from complications of other conditions. They stay up-to-date with the latest advancements in podiatry, allowing them to deliver cutting-edge treatments and techniques.
With over 40 surgeons in our network at The Surgical Clinic, we are confident that our Nashville foot and ankle specialist team can care for each patient with compassion and advanced care. Don’t take another step before you find a board-certified podiatrist near you. We at TSC are your Nashville podiatry experts. Please schedule an appointment with our healthcare team today.
Podiatry Blog in Nashville
Understanding Diabetes and Your Feet
Diabetes, a chronic condition affecting sugar metabolism in the body, has far-reaching implications. Living with diabetes means more than managing blood sugar levels; it involves understanding how this condition can significantly impact various aspects of your health,...
When You Should See a Podiatrist
Podiatry is the medical practice dealing with conditions of ankles and the feet. As a result, a podiatrist in Tennessee is prepared to deal with several medical conditions and provide treatments for them. But when should you see a podiatrist? After all, foot pain may...




